
Full-service care transformation powered by 10+ years of experience, a dedicated clinical workforce, and our AI-enabled platform.

Enroll 10,000 patients in 90 days and start running programs that drive clinical outcomes at scale, from improving medication adherence to reducing readmissions.

Patients demand 24/7 connection. Providing concierge-level care to all your patients is not just feasible; it’s a profitable way to drive better health outcomes.
Phamily is your strategic partner. We drive care transformation by providing proactive care management for all your patients. We combine a decade of experience and dedicated clinical staff with our AI-powered platform to deliver improved patient outcomes and net new cash flow.
Programs like Medicare’s APCM (Advanced Primary Care Management) and other value-based population health models fund the long-term infrastructure that will enhance your financial performance, whether you operate under FFS or VBC models.
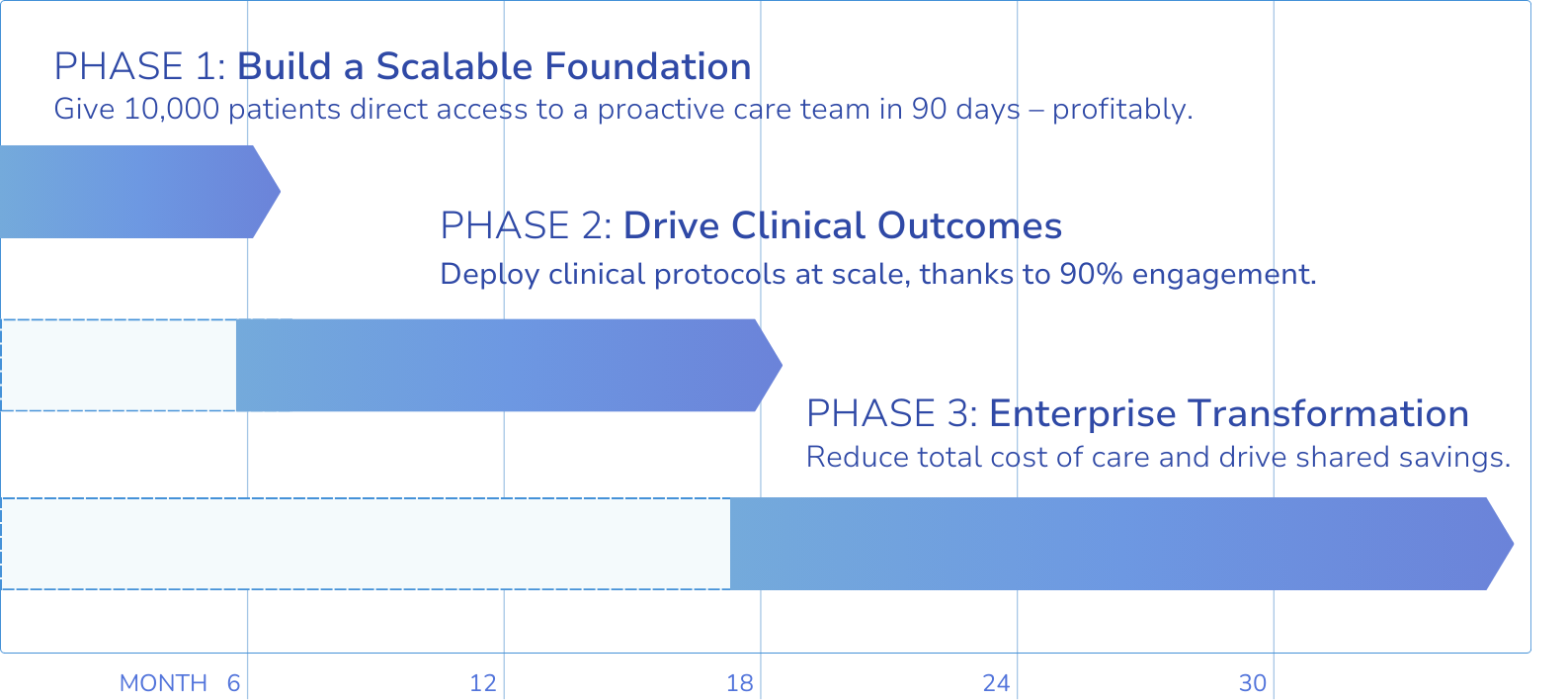
Phase 1 (Months 1-6): Build a Scalable Foundation
Launch with large-scale enrollment (first cohort of 10,000 patients in 90 days). Move labor costs off your balance sheet. Highly-satisfied patients get direct access to a dedicated proactive care team.
Result: Profitable in <90 days. $2.5M Net Operating Income per 10k patients. 83 NPS.
Phase 2 (Months 6-18): Drive Clinical Outcomes
Leverage 90%+ engagement* to steer patients to specific clinical interventions that drive impacts: Close care gaps, drive AWVs, and reduce readmissions.
Example Result: Reduce readmissions by 40%.
Phase 3 (Month 18+): Enterprise Transformation
Manage Total Cost of Care (TCoC) management and maximize shared savings. Roll out concierge-style care management across your entire IDN/CIN.
Result: $1,885 TCoC reduction per patient per year*
Are you a specialty medical group?
Phamily helps leading specialty networks and medical groups support vulnerable populations with high-quality between-visit care management programs.




We deploy a complete care infrastructure—people, process, and purpose-built technology—that acts as a white-labeled extension of your team. We deliver a clinical and financial advantage that is impossible to replicate internally.
Patients get direct access to personalized, concierge-style care management — keeping them healthy and in your network.
We deploy our specialized clinical team and can “badge-flip” your existing underutilized staff. Reduce labor expenses or reallocate staff.
Our team (including APPs, RNs, LPNs, LMSWs, etc.) handles the routine work. Your providers preserve their time for high-complexity care.
Our platform enables us to roll out clinical protocols for tens of thousands of patients (with EHR integration).
Our experienced team becomes an integral part of your organization. Point us at a problem, and we’ll help you solve it.
What would care transformation (that funds itself) look like at your organization?
Let us run a complimentary, custom analysis on your specific patient population to project net operating income, shared savings, and labor efficiency gains.