
At this year’s NeuroNet Pro Annual Summit, one conversation stood out: Neurologists are being compensated unfairly. The numbers prove it, but even more compelling were the discussions with real physicians—people like you—who are feeling the weight of administrative burdens, low reimbursements, and financial pressures that make it harder to stay independent.
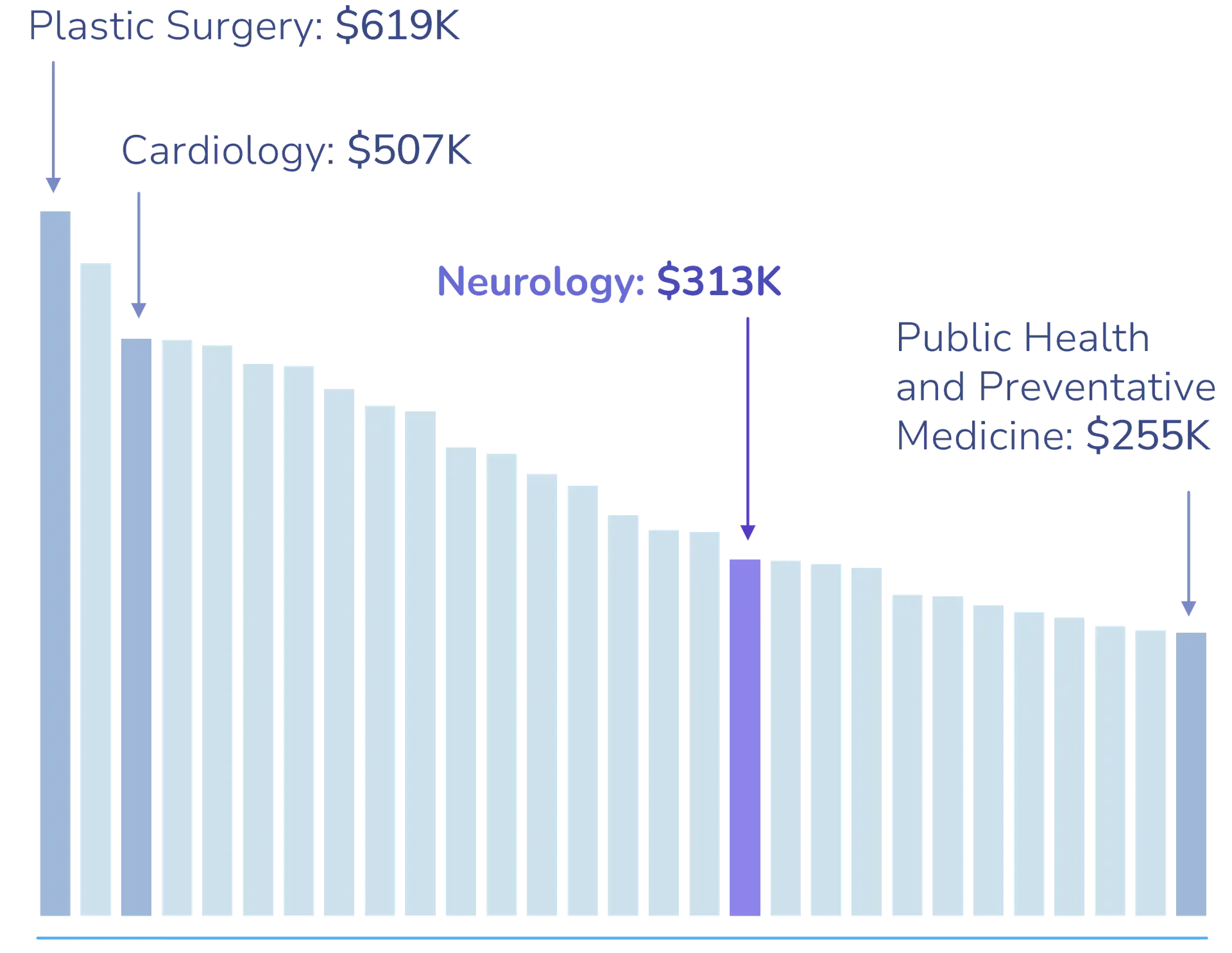
Compared to their peers in other specialties, neurologists often earn significantly less, despite managing some of the most complex cases in medicine. Neurologists earn an average of $313,000 per year, while plastic surgeons make $619,000, orthopedic surgeons $573,000, and cardiologists $507,000.
The reason? Neurology is a cognitive-heavy specialty, meaning fewer billable procedures and a system that rewards interventions over ongoing patient management.
The reimbursement model is not built in your favor, even though neurologists are some of the most essential medical professionals today.
Many neurologists are struggling with the economics of private practice.
During NeuroNet, practice leaders shared just how much these financial pressures and administrative burdens are impacting their ability to run their practices effectively.
The burden of paperwork and compliance is growing, eating into time that should be spent with patients. In fact, physicians spend nearly two hours on administrative tasks for every hour of patient care.
For independent neurologists, this translates into more unpaid work, lower efficiency, and ultimately, a struggle to keep up with patient demand. This administrative overload is also driving consolidation. In 2022, only 46.7% of physicians worked in a fully independent practice, down from 60.1% in 2012.
This financial strain isn’t just a numbers issue—it’s also a well-being issue. Neurologists report working a median of 55 hours per week, compared to 50 hours for all U.S. physicians, and only 32.3% feel they have enough time for their personal lives. Burnout rates continue to rise, making it harder for practices to retain talent and sustain long-term operations.
Rising administrative burdens, declining reimbursements, and increasing competition from larger health systems have made it harder than ever for independent neurologists to stay afloat. The question isn’t just how to survive—but how to thrive while maintaining autonomy.
At NeuroNet, practice leaders shared key strategies that are helping independent neurologists strengthen their financial position while maintaining high-quality care. From bringing services in-house to launching Chronic Care Management (CCM) programs, these solutions are proving effective in keeping practices viable.
Another major takeaway from NeuroNet was how independent neurologists are moving critical services in-house to regain control over patient care and reimbursement.
Several neurologists shared how setting up their own infusion centers helped them deliver high-quality treatments while keeping revenue in-house. Rather than referring patients to hospital systems, practices that establish infusion services can increase patient retention and create a profitable, value-added service.
Independent neurologists at NeuroNet also discussed bringing imaging back into their practices to improve patient care, reduce costs, and retain revenue that would otherwise go to hospitals. One neurologist shared how an in-house imaging center streamlined diagnostics while keeping reimbursements within the practice. Others highlighted how AI-driven neuroimaging solutions are enhancing speed, accuracy, and profitability, helping independent practices compete more effectively, while improving care for patients.
One of the key insights from NeuroNet was that sustaining profitability isn’t just about adding services—it’s about doing so efficiently and at scale.
Group purchasing organizations (GPOs), like NeuroNet, help independent practices lower costs on pharmaceuticals and in-house services such as infusion and imaging. By leveraging a GPO, neurologists can secure better pricing, optimize operations, and boost profitability while maintaining autonomy and control over patient care.
One of the most discussed strategies at NeuroNet was leveraging CCM programs to generate revenue without adding extra workload. Wendy Van Fossen, CEO of The Neurology Center, shared at the event how implementing CCM allowed her practice to get reimbursed for work they were already doing:

“We’re doing this work anyway. We should get paid for it.”
Chief Executive Officer, The Neurology Center
CCM programs offer a sustainable way for neurologists to increase revenue while enhancing patient care. With complex conditions like Alzheimer’s, Parkinson’s, and multiple sclerosis, patients require frequent follow-ups, medication management, and care coordination.
Neurologists at NeuroNet shared how CCM has become a critical tool for sustaining their practices, ensuring high-quality care for patients while securing reimbursement for work they were already doing.
If you’re not leveraging CCM, you’re leaving money on the table—money that could help keep your practice independent.

Independent neurologists are staying competitive by capturing reimbursement for the work they already do (CCM), bringing high-value services in-house (infusions & imaging), and leveraging GPOs to maximize profitability.
If you missed the discussion at NeuroNet, these strategies are helping neurologists thrive—and they’re worth considering for your practice.

Brianne is dedicated to improving the U.S. healthcare system by advocating for better patient care and provider sustainability. With extensive experience in digital health marketing, she focuses on raising awareness of sustainable, high-quality care models and helping providers navigate the shift to financially viable, patient-centered care.

Adam is deeply passionate about utilizing technology and working closely with healthcare providers to improve quality of care and reduce healthcare costs.